gynaecologyat Ruby
- Treating Infertility by Modern and Ayurvedic medicines and Laproscopic Surgeries.
- Diagnostic Laproscopic /Hysterescopy ovarian Drilling.
- Examing Uterine cavity internally and outsides Fallopian Tubes, Ovaries by camera scope.
- Ovarian Drilling – Enhances pregnancy chances in PCOS CASES
- Ovulation Induction & IUI
- Hysterectomy (Uterus Removal)
- Myomectomy (Fibroid Removal)
- Repair for Loosing of vagina , Breast , and Uterus
- Cosmetology – Skin & Hair caring
- Obesity Management.
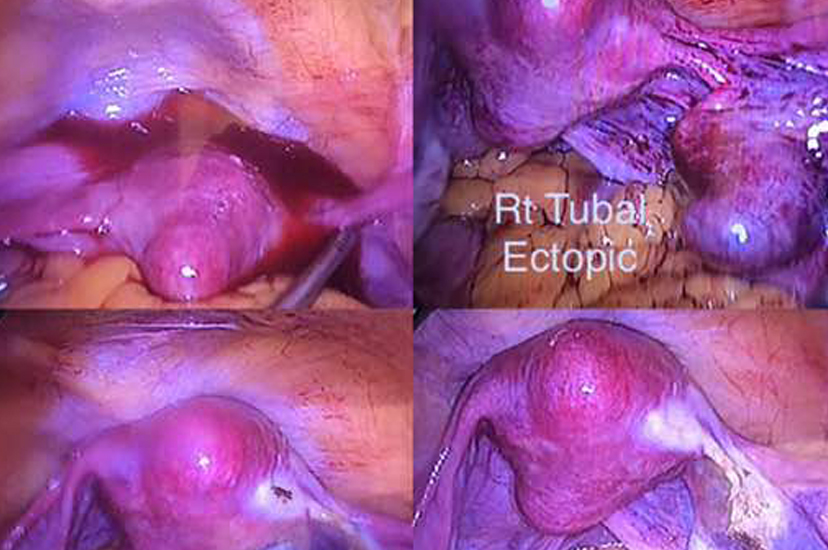
Procedures
Procedures
Hysterectomy
What is Hysterectomy?
In simple words, hysterectomy is a surgical procedure that is carried out to remove the womb or uterus. As the uterus is removed, you will no longer be able to conceive. While all women go through the phase of menopause, some can be faced with symptoms of menopause after undergoing a hysterectomy surgery if the ovaries have also been removed; no matter what their age is. A hysterectomy surgery is commonly recommended by healthcare experts for women with conditions such as multiple fibroids or prolapsed uterus. The extent of this surgery varies widely, depending on the reason for surgery. In some cases, doctors remove the uterus completely, while in some others, they remove both, the ovaries and the fallopian tubes. The fallopian tubes are the structures that help in safe transportation of the eggs from the ovary to the uterus. Leaving the ovaries behind prevents the onset of menopause after the surgery in younger women
What is Hysterectomy?
A hysterectomy is commonly suggested by doctors when other treatment options are not available or have been unsuccessful. Depending on your case history, a hysterectomy surgery is needed if you have:
- Cervix, uterus or ovary cancer
- Multiple uterine fibroids
- Heavy periods
- Endometriosis
- Uterine prolapse
- Adenomyosis
Are There Any Types of Hysterectomy?
There are different types of hysterectomy, which include:
- Partial Hysterectomy - As the name suggests, in a partial hysterectomy, only a portion of the uterus is removed. The cervix is left intact.
- Total Hysterectomy – In a total hysterectomy, the uterus is removed entirely, including the cervix by a health care professional.
- Hysterectomy and Salpingo- Oophorectomy - In this procedure, the uterus along with one or both the ovaries and even the Fallopian tubes are removed. In case both the ovaries are removed, you may need to consider hormone replacement therapy.
How Is Hysterectomy Performed?
A hysterectomy surgery can be performed by a qualified gynaecologist by three different methods. Irrespective of the way in which it is performed, general or regional anaesthetic (spinal or epidural anaesthesia) is necessary.
- Vaginal Hysterectomy - In this type of surgery, a small incision is made inside the vagina to remove the uterus.
- Laparoscopic Hysterectomy - A tiny instrument, which is a long and thin tube, having a high-intensity light and high-resolution camera called a laparoscope is used. Incisions are made in the abdomen, through which, the health care expert cuts the uterus into small pieces to remove it.
- Abdominal Hysterectomy - In an abdominal hysterectomy, an incision is made in the abdomen through which the surgeon performs the removal of the uterus.
Tubectomy
What Is Tubectomy?
Over the years, Tubectomy has become an increasingly prevalent form of contraception in India. Also called as Tubal Ligation, this surgical procedure is carried out to ensure that the fallopian tubes in your body are blocked-clamped, sealed or severed. The main aim of this surgery is to prevent the sperm from reaching the egg to fertilise it. It is a permanent method of sterilisation and there is no going back. Professional surgeons at RUBY HOSPITAL perform this surgery using state-of-the-art facilities.
What Is the Procedure of Tubectomy?
Tubal ligation may be done while you're recovering from vaginal childbirth (using a small incision under the navel called a mini-laparotomy) or during a cesarian or C-section delivery. It can also be carried out as an outpatient procedure (interval tubal ligation) that is separate from childbirth.An interval tubal ligation is usually done with a laparoscope- a thin tube equipped with a camera lens and light- under short-acting general anaesthesia. The complete procedure is carried out in an operation theatre. However, our experts at RUBY HOSPITAL advise that the risk of complications during surgery are higher if you undergo tubal ligation surgery when you have had previous pelvic or abdominal surgery.
Is There Any Way to Reverse the Procedure?
A tubectomy is a permanent form of contraception for women, and there is no going back. It is a permanent method of birth control. However, there are instances where women tend to ask for a reversal. In such a case, surgery will need to be carried out. However, they are not guaranteed of a successful reversal. Some studies have shown that tubal reversal, a microsurgery that reverses the effect of a Tubectomy, has shown a successful reversal. However, the pregnancy rate post the reversal is quite low.
Pap Smear & Colposcopy

Screening tests are an essential part of health care. At RUBY HOSPITAL, we strongly urge our patients to regularly go in for health checkups, to ensure that the signs of cancer can be detected in its earliest stages and make sure that treatment can begin long before the spread of cancer and onset of symptoms. With instances of patients suffering from cancer affecting the breast, ovarian and uterine on the rise, the importance of procedures like a PAP test become immediately apparent.
What Exactly Is A PAP Test?
A PAP test is a simple screening tool that is used to locate the abnormal cells on the cervix. A PAP smear test can help in identifying the abnormalities before the development of the cancer cells. It is a great tool for cervical cancer screening.
Screening with a Pap smear must start every year beginning three years after the first sexual encounter or by age 21 whichever is sooner. After three normal Pap tests, you can lengthen the interval to every three years. However, it must be annually for those at high risk such as those with high-risk sexual lifestyle/partner with high-risk sex lifestyle, those with HPV infection, those on oral contraception for over five years, early marriage, teenage pregnancy, those who smoke. Cervical cancer is unlikely to develop in women over 64 and Pap screening can stop at this age if you have had normal Pap tests in the previous ten years and 3 or more documented standard Pap tests. If you have not been sexually active with a man, your chances of developing cervical cancer are very low, and you may, therefore, choose not to have a screening test.
It's important to remember that, although a cervical smear is the best way to check the health of your cervix, it isn't an absolute test.
Sometimes, screening can show possible signs of cervical cancer when in fact there is no problem. Up to one in 10 cervical smear tests have to be re-taken because of a problem with the test. This can happen if you have an infection, if not enough cells were collected during the smear test or if the cells were hidden by blood or mucus.
The best time to be screened is usually 14 days after your last period. You can't be screened during your period. If you're pregnant - it's usual to wait until three months after you have had your baby.
If minor cell changes were found on your test, you would need to have a repeat screening test - usually in six months. If the repeat screening test is normal, you will be asked to have one more test in the next six to 12 months. If this is normal, you will return to routine testing. If the repeat test still shows the borderline changes, you may be asked to have a colposcopy.
How is the Test Conducted?
A PAP smear procedure is simple and is a routine gynaecological exam. The test or procedure is painless and quick. In this procedure, the cell samples are obtained from the cervix. The cervical cells are then collected using a broom or spatula and a brush. Once the PAP smear for cervical cancer is completed, the cells are sent to a laboratory. To get the best results, our in-house laboratory experts at RUBY HOSPITAL examine the cells minutely under the microscope.
What Exactly is Colposcopy?
Colposcopy procedure is a simple procedure, in which, the doctor uses a magnifying device to have a look at your vulva, vagina, and cervix. This helps in identifying the abnormal cells easily. If a problem is observed during a colposcopy, a biopsy may be taken. One of the benefits is that it helps in examining the external genital area i.e. the vulva, cervix, and the vagina.
The procedure for the test is the same as a PAP test. It is vital to know that a colposcopy procedure is not carried out while you are menstruating. Also, you will be asked by the colposcopy clinic to avoid intercourse, any vaginal medication, tampons or douches 24 hours before the test.

Pain management

Pain medications such as the nonsteroidal anti-inflammatory drugs (NSAIDs) or naproxen may be prescribed to help ease painful menstrual cramps.
Getting regular exercise can help relieve symptoms.
Hormone therapy
Hormone therapy: Supplemental hormones are sometimes effective in reducing or eliminating the pain of endometriosis. It may recur after stopping the course of therapy.
Surgery
Conservative surgery: If you have endometriosis and are trying to become pregnant, surgery to remove as much endometriosis as possible while preserving your uterus and ovaries may increase your chances of success. If you have severe pain from endometriosis, you may also benefit from surgery however, endometriosis and pain may return.
The procedure may be done laparoscopically or through open abdominal surgery in more extensive cases.
Assisted reproductive technologies such as in vitro fertilization, to help you become pregnant are sometimes suggested if conservative surgery is ineffective.
Laparoscopic Hystrectomy
If you have been advised a hysterectomy for any reason such as for fibroids, then laparoscopic hysterectomy is an option that a healthcare expert may suggest. A minimally invasive surgical procedure, a laparoscopic hysterectomy will be performed by an experienced surgeon, in our state-of-the-art centre at RUBY HOSPITAL.
What Is Laparoscopic Hysterectomy All About?
A laparoscopic hysterectomy is a surgery that is undertaken to remove the uterus or womb. Removal of the uterus means that you no longer can conceive. Apart from the uterus, the ovaries, and fallopian tubes may also be removed, and this surgery is called as salpingo-oophorectomy.
How Is Laparoscopic Hysterectomy Performed?
A laparoscopic hysterectomy surgery requires a small or half-inch-long incision in your abdomen. The pelvic region can be clearly seen by inserting the laparoscope (a tube with a light source and a tiny camera that allows your surgeon to see your internal organs) through these incisions. Some instruments are then inserted through the other small incisions in your abdomen or vagina, to remove your womb, the cervix and any other parts of your reproductive system.
Why You Need a Laparoscopic Hysterectomy?
A laparoscopic hysterectomy is performed for numerous health issues. Some of the common problems include:
- Fibroids
- Cervical or womb cancer
- Heavy or irregular periods
What is Total Laparoscopic Hysterectomy?
Total Laparoscopic Hysterectomy (TLH) is an advanced procedure. During a total hysterectomy, your womb and cervix (neck of the womb) are removed. It is also called as a keyhole surgery. It is done using small incisions in your abdomen through which a laparoscope is inserted and other instruments to perform the surgery. In simple words, in this surgery, your uterus is removed completely through the vagina. One or both of the ovaries and fallopian tubes may also be removed.
Benefits of Laparoscopic Hysterectomy
A laparoscopic hysterectomy is associated with less pain as there are only small incisions made in the abdomen. It has a low risk of infection and blood loss. Recovery is fast, and the patient can go home early.
Urinary Incontinence treatment

What Is Urinary Incontinence?
Also known as involuntary urination, Urinary Incontinence is the unintentional passing of urine. It is also commonly referred to as ‘loss of bladder control’. This condition can be embarrassing at times, and is often faced by expecting mothers during pregnancy. The severity of this condition can either range from a few drops of urine leakage while sneezing or coughing to an uncontrollable urge to urinate without being able to get to a toilet in time. While both, men and women can be affected with this condition, it is more commonly seen in females. At RUBY HOSPITAL, we understand how this condition can affect your daily life, and specialise in Urinary incontinence treatments for women.
Types and Symptoms of Urinary Incontinence
There are around four types of Urinary Incontinence commonly seen in patients:
- Stress Incontinence – This type of incontinence occurs when your bladder is under pressure such as when you cough or laugh.
- Overflow incontinence -This type of incontinence is typically faced when you experience frequent or sometimes even constant dribbling of urine, which is mostly due to a bladder that doesn't empty completely.
- Urge incontinence – As the name suggest, in this type of continence, you get an intense and uncontrollable urge to urinate, followed by an uncontrollable loss of urine. Patients suffering from this condition tend to urinate more frequently, and the exact cause of this condition is unknown.
- Functional incontinence – This condition is usually faced by patients who are unable to reach a toilet in time. Patients suffering from conditions leading to immobility or one that interferes with the mental function may face functional incontinence.
Causes of Urinary Incontinence
In women, the most common type of Urinary Incontinence faced is Urge and Stress Urinary Incontinence. Urinary incontinence may have other easily treatable causes such as
- urinary tract infection -Infections can irritate your bladder, causing you to have strong urges to urinate, and sometimes incontinence.
- Constipation-The rectum is located near the bladder and shares many of the same nerves. Hard, compacted stool in your rectum causes these nerves to be overactive and increase urinary frequency.
Urinary Incontinence may be a persistent condition and may be associated with:
- Obesity
- Hereditary
- Pregnancy and vaginal birth- A vaginal delivery can weaken the muscles needed for bladder control and also damage the bladder nerves and supportive tissue. Thus, leading to a dropped (prolapsed) pelvic floor.
- Age- Ageing of the bladder muscle can interfere with the capacity of the bladder to store urine.
- Hysterectomy- During surgery, there may be damage to the supporting pelvic floor muscles, which can lead to incontinence
- Neurological disorders- Parkinson’s Disease, stroke, brain tumour or spinal injury can all interfere with the nerve signals that control the bladder, resulting in incontinence.
Urinary Incontinence Treatment
Our healthcare experts at RUBY HOSPITAL strongly suggest that you take a few simple measures to improve the symptoms of the condition being faced. Improvement can be made, either by changing your lifestyle, losing weight, pelvic floor exercises or even bladder training. According to your case history, there are also certain forms of medications that may be prescribed by our Consultants.
In cases where such measures fail to help, surgical procedures can also be suggested for effective Urinary Incontinence treatment. Treatment for frequent urination that our healthcare experts may recommend include a sling procedure that reduces pressure on the bladder, surgery on the pelvic floor for prolapse, retropubic suspension or tension-free vaginal tape surgery. Schedule a health check-up or an appointment with us to get a detailed diagnosis and advice.
Pelvic Inflammatory Disease

What Is Pelvic Inflammatory Disease?
Pelvic inflammatory disease (PID) is an infection of the female reproductive organs, usually caused by a sexually transmitted infection (STI). If left untreated it can cause infertility. PID can also result in the case of an infection that spreads from the vagina and cervix (neck of the womb) to the womb (uterus), ovaries and fallopian tubes (the tubes that go from the ovaries to the womb). PID can become a long-term health problem and can regularly flare up and affect the quality of your life.
At RUBY HOSPITAL, our healthcare professionals are experienced in diagnosing and providing the treatment for pelvic inflammatory disease. While there is no single test to diagnose PID, our doctors will diagnose you on the basis of your symptoms and a gynaecological examination. Schedule an appointment with our healthcare givers to ensure that you get a prompt diagnosis and treatment if needed.
Symptoms of Pelvic Inflammatory Disease
Symptoms associated with Pelvic Inflammatory Disease tend to vary. However, some of the common symptoms include:
- Irregular periods
- Pain in the lower abdomen
- Painful sex
- Pain during urination
- Chills or high fever
- Vomiting
- Nausea
- Vaginal discharge accompanied with foul smell
- Back pain
- Fatigue
- Diarrhea
Impact of Pelvic Inflammatory Disease
PID is also one of the primary preventable causes of infertility. If you do not receive treatment for your pelvic infection in time, you may have flare-ups of the disease, or you could have an ectopic pregnancy (when the pregnancy occurs outside the uterus such as in the fallopian tubes). If a pregnancy occurs, it may be associated with complications such as a preterm pregnancy or passing on the infection to your newborn.
Who Is at Risk of Pelvic Inflammatory Disease?
Some factors put a woman at risk for Pelvic Inflammatory Disease. Patients who are most at risk for this condition include:
- Women who have had Pelvic Inflammatory Disease earlier
- Women with Sexually Transmitted Diseases (STD)
- Women with many sexual partners are prone to STD and ultimately PID
- Teenagers who are sexually active
Pelvic Inflammatory Disease Treatment
Mild cases of Pelvic Inflammatory Disease can be treated by antibiotic medication is taken orally. Severe cases, though, may require a combination of oral and intravenous antibiotics.
In case you have symptoms of nausea, high fever or vomiting, or you have symptoms that mimic an ectopic pregnancy, you might need to be hospitalised for a detailed examination. A pelvic exam will be performed that will confirm the tenderness in the pelvis. The exam will also help in identifying the location of the infection. Suitable treatment of PID will be started after swabs of your vagina and cervix are sent for examination.
It is essential to take the full course of antibiotics to cure the infection completely.
You may be advised a surgical procedure such as laparoscopy to confirm the diagnosis and also to deal with any adhesions that may have resulted from the infection and contribute to infertility.
Prolapse treatment
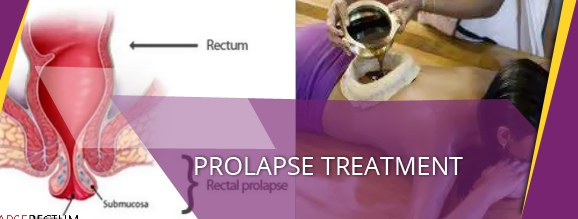
Pelvic organ prolapse or Prolapse is a condition that often may not cause any symptom. It is essentially a condition in which one or more of your pelvic organs may bulge into the vagina. A prolapse can occur at any time and any age. There are types of prolapse, which differ according to which organ is affected and of varying degrees that may be staged from 1 to 4 with 4 indicating a severe prolapse. Depending on the condition, the right prolapse treatment may be prescribed. It is important to note, though, that when this condition is detected early, it can be treated non-surgically. Thus, it is essential that you take the advice of your doctor at the earliest if you feel that you may be suffering from this condition.
What is Prolapse All About?
In women, a prolapse refers to the pelvic organs bulging into the vagina. This may be an anterior prolapse (cystocele), where the bladder bulges in the front part of the vagina; or a prolapse of the uterus and cervix on top of the vagina or posterior wall prolapse (rectocele or enterocele) where the bowel bulges into the vagina. Prolapse is caused by a weakening of tissues that support the pelvic organs. Though there is rarely any one cause, there are conditions that predispose to it developing, such as older age and the onset of menopause, being overweight, having had a previous difficult labour and delivery, a previous hysterectomy, doing manual work that involves straining and chronic constipation. Pregnancy hormones can cause ligaments to stretch and relax, and the extra weight during labour and delivery can strain the pelvic floor and weaken it.
Symptoms of Prolapse
The symptoms associated with a prolapse vary, depending on how severe it is. If it is a minor prolapse, it is not noticeable. However, a severe prolapse can cause symptoms that include:
- Lump or a bulge in the wall of the vagina which may need to be pushed back in severe cases
- Dull lower back pain
- Discomfort or aching in the pelvic region
- Constipation
- Sexual problems
- Urinary stress incontinence
Prolapse Treatment
Many women with prolapse don't need treatment and lifestyle changes such as weight loss, and pelvic floor exercises are recommended in mild cases.
In severe cases, a prolapsed uterus surgery is required that will correct the defect that resulted in the prolapse. It is a relatively simple procedure in which a gynaecologist will make an incision in your vagina and stitches are placed so that the support that is provided by the pelvic floor muscles to the pelvic organs is improved. Surgery may also involve a hysterectomy in some cases, especially where the uterus has prolapsed out.
Can a pelvic prolapse be prevented?
Lifestyle changes will help to avoid a prolapse. Maintain a healthy weight, exercise regularly, do pelvic floor exercises and avoid smoking. Prevent constipation with a high fibre diet that includes adequate water and avoid heavy lifting.
Menorrhagia treatment

Are you experiencing heavy periods that last much longer than what is acceptable? Menorrhagia is the term used to describe the condition in which several regular heavy periods occur that affect you physically and emotionally.
What Is Menorrhagia?
It is very difficult to measure the amount of blood lost during a period so generally, heavy periods is diagnosed when,
- You need to change your sanitary towel frequently-every two hours or earlier or need to use additional protection
- You pass blood clots and often stain your clothes or bed linen at night
- The heavy periods affect your regular life-work and regular activities
What Are the Causes of Menorrhagia?
In about half the women with Menorrhagia, the cause cannot be detected, and the term Dysfunctional Uterine Bleeding (DUB) is used to describe this condition. When there is a cause that exists, it may be one of the following:
- Uterine fibroids
- Uterine polyps
- Cancer of the uterus
- Polycystic ovarian disease (PCOD)
- Endometriosis
- Pelvic inflammatory disease (PID)
- Having an intrauterine contraceptive device (IUCD) implanted
- Blood disorders
What Are the Signs and Symptoms of Menorrhagia?
The duration of a normal menstrual cycle typically is between three to five days. In cases where patients suffer from Menorrhagia, periods tend to last for more than seven days and are associated with excessive blood loss and excessive clots being passed.
The effects of menorrhagia are related to the lack of red blood cells and iron deficiency that results. About two-thirds of women with menorrhagia have iron deficiency anaemia that manifests as fatigue, tiredness, and shortness of breath.
Tests & Treatment for Menorrhagia
Menorrhagia treatment completely depends on factors that include your overall clinical condition, whether you plan to have children in future, the severity of the menorrhagia and whether a cause has been detected.
Your doctor will typically do a physical exam, and recommend other procedures such as blood tests, a PAP smear, an ultrasound scan and in severe cases, an endometrial biopsy. Depending on the results of your initial tests, your doctor may recommend that you undergo further testing that may include procedures like a dilatation and curettage (D & C), a hysteroscopy or a laparoscopy.
Treatment options include non-steroidal anti-inflammatory drugs (NSAIDs), the combined oral contraceptive pill, iron supplements to treat the anaemia and tranexamic acid. You may be recommended a levonorgestrel-releasing intra-uterine system (IUS)-Mirena®. This will be recommended only if you agree to have it fitted for at least a year. The IUS lasts up to five years and should help to improve your menorrhagia within the first three to six months
Some of the other treatment options are
- Uterine artery embolization that will reduce the blood flow to any fibroids causing them to shrink
- Endometrial ablation, where most of your womb lining is destroyed or removed using energy such as microwaves or heat.
- Myomectomy is the surgical removal of uterine fibroids
- Hysterectomy is usually only done if other treatments haven't worked. After a hysterectomy, you will no longer have periods and won't be able to become pregnant.
Get in touch with our team of healthcare professionals to get a better understanding of this condition, as well as an accurate diagnosis of the same.
Premenstrual Syndrome treatment (PMS)
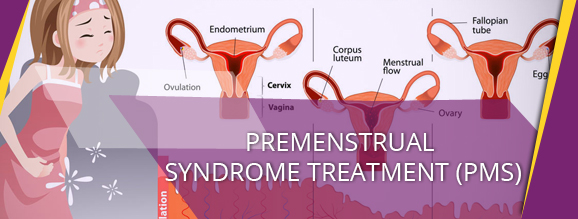
Premenstrual Syndrome (PMS) is a condition that is common in young and middle-aged women, and as many as three out of every four women have experienced it at some point in their life. The symptoms for this tend to recur in a predictable pattern linked to one’s periods, and the spectrum of emotional and physical changes experienced can range from slightly noticeable to severe.
Symptoms may be related to emotional changes and physical symptoms and in some women, the symptoms may impact their lifestyle and relationships. To control the condition of Premenstrual Syndrome in your life, it is important that you consult a doctor who will advise you regarding the different treatment options and lifestyle adjustments that may help.
What is Premenstrual Syndrome (PMS) all about?
As the name suggests, Premenstrual Syndrome (PMS) are symptoms that a woman faces, typically starting a week or more before her period is due. The symptoms aren't unique to PMS, but it is the timing of the symptoms that suggests the condition. The symptoms get better once her period has started and it recurs each month.
While the cause of this condition is still not clear, it is believed to be related to fluctuations in a woman’s hormonal levels.
Symptoms of Premenstrual Syndrome (PMS)
The symptoms of premenstrual syndrome tend to vary from one woman to another. Some of the common symptoms include:
Emotional symptoms: These include symptoms such as confusion, depression, angry outbursts, fatigue, stress, moodiness, irritability, insomnia, crying spells, inability to concentrate, social withdrawal and lack of confidence.
Physical symptoms: These include symptoms such as breast tenderness, muscle and joint pains, feeling bloated, headaches, acne, change in appetite and abdominal pain.
Easing Premenstrual Syndrome (PMS) symptoms
Symptoms of premenstrual syndrome can be tackled with simple-to-follow routines like:
- Drinking lots of water
- Incorporating a balanced diet that is rich in fibre, vegetables and fruit and low in salt, sugar and caffeine
- Exercising regularly
Premenstrual Syndrome treatment (PMS)
Treatment for Premenstrual Syndrome (PMS) depends on whether you experience mild or severe symptoms. If the symptoms are mild, you can get relief by making changes to your lifestyle or diet. However, if the symptoms are not relieved, it is advisable to get in touch with a healthcare expert at a facility like RUBY HOSPITAL to get treatment.
While most symptoms of PMS are reduced with the start of your periods, the condition may be associated with disabling symptoms each month. Such cases of PMS are called premenstrual dysphoric disorder (PMDD), and will require the help of a medical professional. As part of the treatment for PMS, our doctors at RUBY HOSPITAL will collect the necessary details about your clinical history of depression and mood disorders related to your periods. Also, other tests like a thyroid function test and a pregnancy test may be advised, and a pelvic exam will be carried out. Medicines that may be prescribed and are sometimes helpful are the combined oral contraceptive pill, progesterone or a diuretic that will help reduce the bloating.
Contraceptive Device Insertion

Today, most couples, to effectively plan their families, are adopting different methods to prevent pregnancy. An effective device that helps with this is a form of birth control called intrauterine contraceptive device (IUCD) or an intrauterine device (IUD). This method of contraception acts by preventing the sperm and egg from surviving in the uterus or fallopian tubes or even by preventing a fertilised egg from implanting in the uterus.
What is an Intrauterine Contraceptive Device?
Also known as an Intra Uterine Device (IUD), this is a small T-shaped plastic and copper device that is inserted into the uterus and can be left inside for five to ten years depending upon the type. There are different IUDs available, some with more copper than others. Some variations of this device also release hormones that prevent women from ovulating.
A thread is attached at the end of the device, which hangs down through the cervix and into the vagina. It is essential to note, though, that the device should only be inserted and removed by a trained medical practitioner.
How Does the Intrauterine Contraceptive Device work?
Patients often confuse this device with the Intrauterine System (IUS). Instead of releasing the hormone progestogen like the IUS, the IUD releases copper. Copper acts to change the composition of the fluids in the uterus and fallopian tubes so that sperm cannot survive there. IUDs may also stop the fertilised eggs from implanting in the uterus.
IUDs with more copper are more effective than those with less copper. The Intrauterine Device can be put in at any time during the menstrual cycle, as long as the woman is not pregnant. After an Intrauterine Device (IUD) is inserted, the periods may become heavier or longer. This effect may last up to six months, but will settle down. At RUBY HOSPITAL, Intrauterine Device insertion is a procedure that is routinely performed by our experienced Consultants.
Benefits of the Intrauterine Contraceptive Device Insertion
An Intrauterine Contraceptive Device offers some benefits to the woman. Some of them include:
- It is an effective contraceptive method with a failure rate of one percent.
- It is an excellent option for women who are looking for a lasting contraceptive method that is reversible.
- Once the IUD is removed, your fertility gets back to normal immediately

Health Check
Health Check

Teens
Adolescence, while being an extremely vulnerable phase of life, is also the foundation for audulthood. It is most vital then, to monitor the physical, social, emotional and mental development of a teenager. Women Health teens is designed as a comprehensive health check for girls in the age group of 13 to 19 years to address all these concerns sensitively.
Women’s health risks change with her age. However, it is important to realize that your lifestyle choices can go a long way towards reducing your health risks.
Age-specific physiological and emotional changes are more pronounced in women.
There are many health concerns that women have, from concerns about the risks of developing cancer, to issues with weight gain. Keeping in mind that every age group has its own set of health issues, RUBY HOSPITAL offers customized health checkups for women of every age.
W-Health Check - Teens
- CBC
- Blood Group & Rh typing
- Chest X-Ray
- Urine routine tests
- Fasting Blood Sugar
- Post Prandial Blood Sugar
- Ultrasound scan-whole abdomen
- Physician Consultation
- Stool routine tests
Twenties
For young women in their twenties, the possiblity of wedding bells ringing is quite high. Pre-marital screening can help prepare and gear you up for healthy motherhood. RUBY HOSPITAL Royale's Women Health Twenties addresses these and many other issues, and guides you along the path of well-being.
Women’s health risks change with her age. However, it is important to realize that your lifestyle choices can go a long way towards reducing your health risks.
Age-specific physiological and emotional changes are more pronounced in women.
There are many health concerns that women have, from concerns about the risks of developing cancer, to issues with weight gain. Keeping in mind that every age group has its own set of health issues, RUBY HOSPITAL offers customized health checkups for women of every age.
W-Health Check - Twenties
- CBC
- Blood Group & Rh typing
- Chest X-Ray
- Urine routine tests
- Fasting Blood Sugar
- Post Prandial Blood Sugar
- Ultrasound scan-whole abdomen
- Blood Urea Nitrogen
- SGPT
- SGOT
- Serum Creatinine
- Serum Calcium
- TSH
- ECG
- Pap Smear
- Physical Examination
- Gynaec Consultation
- Stool routine tests
Thirties
The Stable career you have built through sheer hard work may prove to be a sress avalanche. Your body is in a state of physical flux, with skin tone problems, bone loss, weight gain and reproductive issues manifesting themselves. Ruby Hospital's Women Health Thirties helps you to continue enjoying wellness of mind and body while building the foundation for good health over many decades.
Women’s health risks change with her age. However, it is important to realize that your lifestyle choices can go a long way towards reducing your health risks.
Age-specific physiological and emotional changes are more pronounced in women.
There are many health concerns that women have, from concerns about the risks of developing cancer, to issues with weight gain. Keeping in mind that every age group has its own set of health issues, RUBY HOSPITAL offers customized health checkups for women of every age.
W-health Check - Thirties
- CBC
- Blood Group & Rh typing
- Chest X-Ray
- Urine routine tests
- Fasting Blood Sugar
- Post Prandial Blood Sugar
- Ultrasound scan-whole abdomen
- Blood Urea Nitrogen
- Lipid Profile
- SGPT
- SGOT
- Serum Creatinine
- Serum Calcium
- TSH
- ECG
- Pap Smear
- Physical Examination
- Gynaec Consultation
- Stool routine tests
Forties
40s are generally considered the mid-point of our lives. Sresss of career and family peak around this time and then there are the shifting hormonal tides. Ruby Hospital's Women Health Forties alerts you to the needs of your body during this transitional decade, and helps you age gracefully.
Women’s health risks change with her age. However, it is important to realize that your lifestyle choices can go a long way towards reducing your health risks.
Age-specific physiological and emotional changes are more pronounced in women.
There are many health concerns that women have, from concerns about the risks of developing cancer, to issues with weight gain. Keeping in mind that every age group has its own set of health issues, RUBY HOSPITAL offers customized health checkups for women of every age.
W-Health Check - Forties
- CBC
- Blood Group & Rh typing
- Chest X-Ray
- Urine routine tests
- Fasting Blood Sugar
- Post Prandial Blood Sugar
- Ultrasound scan-whole abdomen
- Blood Urea Nitrogen
- Lipid Profile
- SGPT
- SGOT
- Serum Creatinine
- Serum Calcium
- TSH
- ECG
- Pap Smear
- Physical Examination
- Gynaec Consultation

Specialty Clinics
Specialty Clinics
Fertility

Conception occurs when a woman’s egg is fertilised by a man’s sperm and implants itself in the uterus. In most couples, conception will occur naturally, while others may require medical intervention to induce conception. In cases where medical intervention is needed, our expert physicians at RUBY HOSPITAL work with you to develop a treatment program that meets your needs, and which will help to maximise your chance of success. With the right management and state-of-the-art treatment facilities, we at RUBY HOSPITAL work round the clock to give you the support you need.
Ovulation and fertility
For women, fertility is determined by ovulation. Hence, the best time to try and conceive is during the ‘fertile window’ of your menstrual cycle. However, this cycle is not always consistent on a monthly basis, therefore making it difficult to determine the exact date of ovulation reliably. At RUBY HOSPITAL, our Fertility clinic staffed with skilled specialists and medical personnel offers diagnostic testing and evaluation so that you have most likely dates in your ovulation cycle. Once your ovulation cycle is determined, it is advisable to have intercourse in the three days leading up to and including ovulation.
Boost fertility
If natural conception does not occur, you can improve your fertility and the chances of conception with a few simple steps. Being underweight or overweight, for example, can delay the time it takes to conceive. Maintaining a healthy weight can boost your chances of conceiving. Consuming too much coffee or alcohol can also impair your fertility. It is advisable to speak with an expert to understand what lifestyle changes you should adopt to help you conceive. Our medical staff at RUBY HOSPITAL, one of the best fertility clinics in India, will help provide you with the ideal natural solution to set you on the path to motherhood.
Dealing with infertility
A lifestyle of sedentary habits, an unhealthy diet, stress, smoking and alcohol intake is one of the leading causes of infertility. When there is a failure to conceive, even after regular intercourse for more than a year, there is a high possibility that either you or your partner is suffering from infertility. Factors such as an unfavourable medical history, genetic disorders or unhealthy lifestyles can affect your ability to conceive. The causes may be related to anatomical, functional, hormonal or psychological reasons. At RUBY HOSPITAL, we recommend that you get in touch with our fertility clinic to understand the best solution, with options such as surgery or In Vitro Fertilization (IVF) that you can explore based on your doctor’s advice.
Fibroids
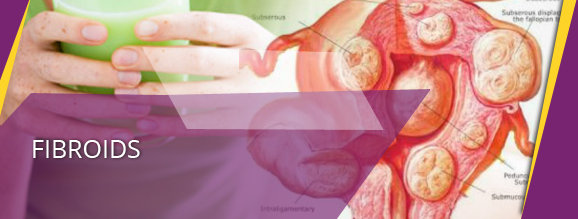
Are you experiencing heavy bleeding between or during your periods, pain in the pelvis or lower back? Symptoms such as this, or others like feeling pressure or fullness in the lower abdomen, may indicate that you are suffering from a disorder called fibroids. This condition requires the immediate attention of a specialised fibroid clinic, like RUBY HOSPITAL, where our skilled team of experts offers you the best treatments available for treating fibroids.
What Are Fibroids?
Fibroids are abnormal growths that develop within or on the uterus, leading to immense pain or a heavy menstrual cycle. In most cases, these tumours are benign, but at some point in time, they can disrupt your menstrual cycle and cause fertility issues, and eventually need to be removed. Although there is no precise reason as to why this disorder occurs, some of the contributing factors include hormonal imbalance, family history, and pregnancy. An imbalance of the oestrogen and progesterone hormones, cause the uterine lining to regenerate, and may overstimulate the growth of fibroids in each menstrual cycle. Another contributing factor to this disorder is family history.
If the disorder runs in your maternal line’s case history, there is a high chance of you developing this disorder. Pregnancy contributes to the increase in the production of oestrogen and progesterone hormones, thus contributing to the development and abnormal growth of fibroids. The medical staff and state-of-the-art diagnostic equipment at our fibroid centre at RUBY HOSPITAL will help you with the right diagnosis as well as the ideal treatment for the same.
To understand if you are suffering from fibroids, you will first need to recognise its indicative signs. Symptoms of this disorder included heavy bleeding between or during periods, excessive blood clots, pain in the pelvis or lower back and increased menstrual cramping. You may also experience an increase in urination, pain during intercourse or even a swelling or enlargement of the abdomen.
Menopause

What is menopause?
Menopause is a natural process, and not a medical problem or illness. After a certain age, women produce lower levels of the hormones oestrogen and progesterone. At this stage, all reproductive functions stop naturally, thus reducing your ability to conceive or get pregnant. While most women undergo menopause naturally, without any side effects, others can suffer from moderate to extreme side effects. Due to changes in hormone levels, menopause in some cases can lead to other health complications. At RUBY HOSPITAL’s Menopause Clinic, we are well equipped and trained to help you through this natural process, and will treat any complications resulting from menopause.
At what age does menopause occur?
The developments leading up to menopause happen over several years, commonly from your early 40s to around 55 years of age. No signs or predictions can indicate when a woman will begin feeling the symptoms of menopause, or even undergo menopause. It starts when your periods become irregular and when you have not had a period for a full year, it is considered as the beginning of your menopause. It should also be noted that the age at which a woman starts experiencing menstrual periods also does not relate to the onset of menopause.
"Induced" or "surgical" menopause happens when a woman goes through an immediate and premature menopause. This occurs when her ovaries no longer produce the hormones oestrogen, progesterone and testosterone and occurs when she has had surgery to remove the ovaries or chemotherapy or radiation treatment. The symptoms are usually more severe.
What are the symptoms of menopause?
Common indicators and symptoms of menopause include weight gain, pain in the joints, vaginal dryness and urinary tract infections. Changes in texture or dryness of the skin, dryness or loss of scalp hair are also common. In some cases, women going through menopause may also observe a reduced sex drive or sexual dysfunction, fatigue, night sweats and osteoporosis. Other commonly reported symptoms include feeling cold, hot flashes, sweating, early awakening, insomnia, or sleeping difficulty. You can also go through emotional symptoms such as anxiety or nervousness, sadness, sense of loss or even depression. In most cases, these symptoms will lessen or disappear once a woman has completed menopause.
PCOS
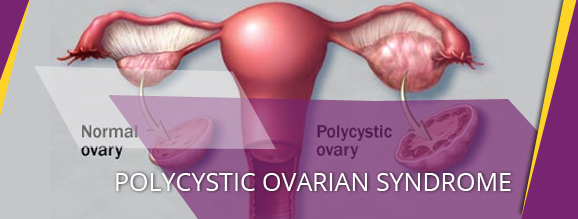
What Is Polycystic Ovarian Syndrome (PCOS)?
Also called as Stein-Leventhal Syndrome, PCOS is a common hormonal problem experienced by women. Most women, who suffer from PCOS, grow cysts on their ovaries. The cysts themselves are not harmful. However, they result in hormonal imbalances. Over time, if this disorder is not treated promptly, can lead to serious health problems, such as diabetes and heart disease.
PCOS cannot be diagnosed by a single test. Your doctor will talk to you about your medical history, conduct a physical exam, and run an ultrasound and blood tests to pinpoint the disorder. As symptoms tend to vary from case to case, it is important that you take the help of an experienced doctor, who will be able to thoroughly diagnose your case before recommending any treatment.
Causes of Polycystic Ovarian Syndrome (PCOS)
The exact cause of PCOS is still unknown. However, research suggests that genes may play a role in this disorder. In case your mother or sister has a history of PCOS, it is advisable to visit a PCOS centre on a regular basis, to ensure that any potential complications are arrested immediately.
Another possible cause may be hormonal changes in your body. The sex hormones lose balance. Normally, the ovaries make a small quantity of male sex hormones (androgens). In PCOS, they start making slightly increased androgens.
The body may have a problem called insulin resistance where it is unable to utilise insulin, When the body is unable to utilise insulin, blood sugar levels go up. Over time, this increases your chance of getting diabetes.
Low-grade inflammation - Your body's white blood cells produce substances to fight infection in a response called inflammation. Research shows that women with PCOS have low-grade inflammation and that this type of low-grade inflammation spurs polycystic ovaries to produce androgens.
Symptoms of Polycystic Ovarian Syndrome (PCOS)
The symptoms associated with PCOS tend to start slowly. In most cases, symptoms begin surfacing when you are in your early teens, around the time when you begin menstruating. Symptoms of PCOS can become more pronounced after a sudden weight gain in this age group.
While the exact signs of this disorder vary from one woman to another, the most common symptom among women is irregular periods, varying from few or no menstrual periods to heavy, irregular bleeding.
Other commonly seen symptoms include:
- Acne or oily skin
- Hair loss from the scalp.
- Pelvic pain
- Infertility, due to inability to ovulate properly, or repeat miscarriages.
- Weight gain.
- Depression or mood swings.
- Breathing problems while sleeping.
- Anxiety
Other than this, certain male characteristics may also begin to develop and may be interpreted as symptoms of PCOS. This includes:
- Thin hair
- Deeper voice
- Extra hair on the face and body. Often women get thicker and darker facial hair and more hair on the chest, belly, and back.
- Decrease in the breast size
Diagnosis of Polycystic Ovarian Syndrome (PCOS)
It is important to note that there is no specific diagnosis designed for PCOS. However, to ensure that you get the best diagnosis, our doctors at RUBY HOSPITAL’s PCOS centre will closely review the symptoms that you are experiencing, and also your medical history. A physical and pelvic exam will also be conducted, to pinpoint any other symptoms or signs that are associated with PCOS.
Polycystic Ovarian Syndrome Treatment
It is vital for a person suffering from PCOS to seek medical advice immediately. While there is no permanent cure for PCOS, this disorder can be tackled with simple lifestyle modifications and medical management. Abstaining from smoking, a healthy diet, weight control, regular exercise can all help you treat PCOS.
You can also be prescribed by doctors to take medication to balance out your hormones. The treatment prescribed will depend on your symptoms, and whether you plan to have a child or not. Constant monitoring of PCOS can help reduce risks like infertility, miscarriages, diabetes, heart disease and uterine cancer.
For women who are faced with adverse symptoms, or are planning to have a child, common treatment procedures prescribed at Polycystic Ovarian Syndrome Clinics include:
- Birth Control Pills: These pills help in controlling the menstrual cycles, reduces the male hormone levels, helps in clearing the acne, and more.
- Fertility Treatments: Research suggests that women suffering from PCOS due to constant hormonal imbalance, can suffer from infertility. Thus, many fertility treatments are offered such as in-vitro fertilisation, ovulation cycles and more.
In extreme cases of this disorder, your doctor may also suggest that you undergo surgery. Some of the commonly prescribed procedures include:
- Ovarian drilling
- Cyst Aspiration
- Hysterectomy
- Oophorectomy
Breast Cancer
Breast cancer is a fear that many women have. It occurs when abnormal cells grow out of control in one or both breasts. They can invade nearby tissues and form a lump, called a malignant tumor. The cancer cells can spread to the lymph nodes and other parts of the body.
When should you get breast screening done?
Breast screening is a simple way to detect early breast cancers, when they are too small for you or your doctor to see or feel. The first stage of breast screening is a mammogram, which is an x-ray of each breast.
For women not at high risk: Get a mammogram done every year beginning from age 40 and older and continue to do so as long as they are in good health. (American Cancer Society guidelines).
The USPSTF (US Preventive Services Task Force) guidelines recommend starting at age 50 and getting it done every 2 years. You should speak to your doctor and decide on the best course for you.
Women in their 20s and 30s should have a clinical breast exam (CBE) done as part of a regular check-up by a doctor, preferably every 3 years
Women should know how their breasts normally look and feel and report any breast change to a doctor right away. Breast self-exam (BSE) is an option for women starting in their 20s. Talk to a doctor about the benefits and limitations of BSE. Women can easily miss a breast lump that an expert can find.And for the same reasons, it is better to learn BSE from an expert.
Some women at high risk for breast cancer – because of their family history, a genetic tendency, or certain other factors – should be screened with MRIs along with mammograms.
If a lump is found, your doctor will evaluate it with an ultrasound of the breast. If required may advise either an FNAC (an examination of the cells aspirated from the lump-an outpatient procedure) or a biopsy.
